
A person inhales these medications and they reduce symptoms by relaxing the muscles around the airways. 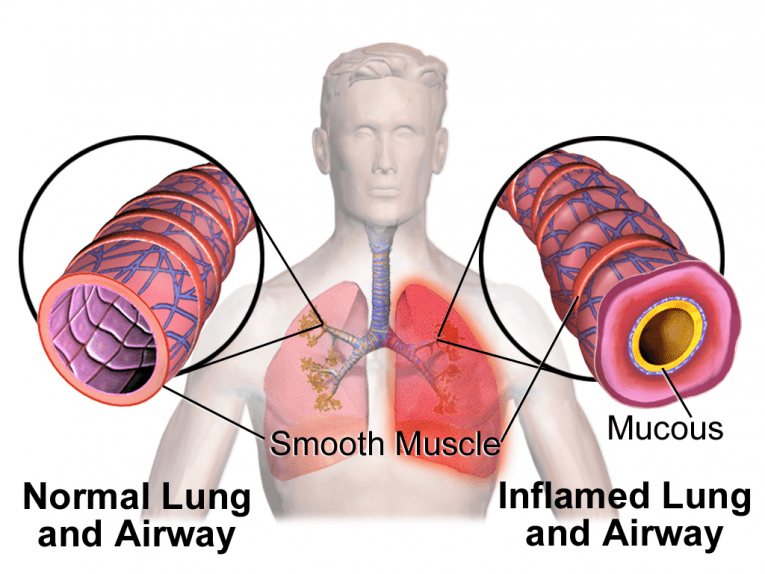
Generally these medications are known as short-acting beta agonists (SABA). Quick-relief medicationsįast-acting drugs control asthma attacks as they happen. They may also add a long-acting beta agonist (LABA) if inhaled corticosteroids aren’t sufficient. Once a medical professional has determined the severity, they will prescribe medications progressively, keeping inhaled corticosteroids as the foundation of treatment. People with infrequent nocturnal asthma symptoms can use a short-acting, inhaled beta agonist medication for quick relief of symptoms.įor people who have nocturnal asthma symptoms one or more times a week, treatment will look similar to normal asthma treatment, and it is tailored to the severity of a person’s asthma. It is also important that people address any underlying disease that can make nocturnal asthma worse, such as rhinosinusitis, heartburn, and sleep apnea. The ALA recommends people with asthma visit a doctor annually to review and potentially revise their asthma treatment plan. The main treatment goals are finding an effective medication and reducing exposure to allergens. Those professionals can assist in creating an asthma action plan to control and treat symptoms as they appear. Individuals should talk with a doctor, allergist, or pulmonologist, which is a respiratory specialist, for advice and treatment options. This is a sleep study that takes place in a laboratory setting. If the doctor suspects obstructive sleep apnea, a condition where an individual stops breathing for brief periods of time during their sleep, then the doctor may order polysomnography (PSG). Parents should monitor their children for symptoms such as wheezing, daytime sleepiness, disturbed sleeping, and difficulty concentrating in school.ĭoctors usually diagnose nocturnal asthma with at-home testing, such as the PEF meter discussed above. Nocturnal asthma often goes undiagnosed in children because they tend to conceal or downplay their symptoms. Because of this, it is important that doctors diagnose and treat nocturnal asthma in children accurately. The negative effects of nocturnal asthma can worsen behavioral and developmental difficulties in children. It is the most common chronic disease diagnosed in children. bedroom allergens like dust mites, pet hair, or moldĪccording to the World Health Organization (WHO), asthma is more common in children than adults.Some general triggers for nocturnal asthma include: Doctors do not fully understand the connection between obesity and asthma, but excess fat around the throat and general inflammation in the body may increase the risk. Obesity is another factor that increases the risk of nocturnal asthma. Individuals who get less than 6 hours of sleep every night have 1.5 times more asthma attacks than those who get the recommended 7 to 9 hours of sleep. A lack of sleep causes inflammation in the body and affects lung function, increasing the chance of an asthma attack. Some individuals experience insomnia during pregnancy. The levels of these hormones fluctuate on a nightly basis, which can cause inflammation in the airways, increasing the risk of nocturnal asthma symptoms.Īccording to the American Lung Association (ALA), hormonal changes that occur during pregnancy can also influence asthma symptoms. Hormones, such as cortisol, epinephrine, and melatonin, all have circadian rhythms, which are the body’s internal 24-hour cycles. While doctors do not fully understand why some people’s asthma worsens at night, some think it may be linked to neurohormonal changes. It is important to note that even if a person does not have PEF variability, they may still have nocturnal asthma. If the difference between the measurements is greater than 15%, the individual likely has nocturnal asthma. However, it is also useful for a person to take their PEF measurements if they wake up during the night. PEF is typically first thing in the morning and again before bed. By using a simple device called a peak expiratory flow (PEF) meter, a person can take measurements of airflow during the day and at night. According to one study, peak lung function occurs at 4 p.m., while minimal lung function occurs at 4 a.m.ĭoctors can determine if someone has nocturnal asthma by looking at their changes in lung function. They may have worsening lung function and increased airway sensitivity.Ī healthy individual’s lung function varies throughout the day. Sometimes, the emergence of nocturnal asthma means a person has severe asthma, or poor control over their symptoms. This can negatively affect sleep quality. Nocturnal asthma means that a person’s asthma symptoms worsen at night. Even minor triggers and allergens can cause those airways to constrict. Share on Pinterest Rubén Carbó/EyeEm/Getty ImagesĪsthma is a condition that causes continuously inflamed airways.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
